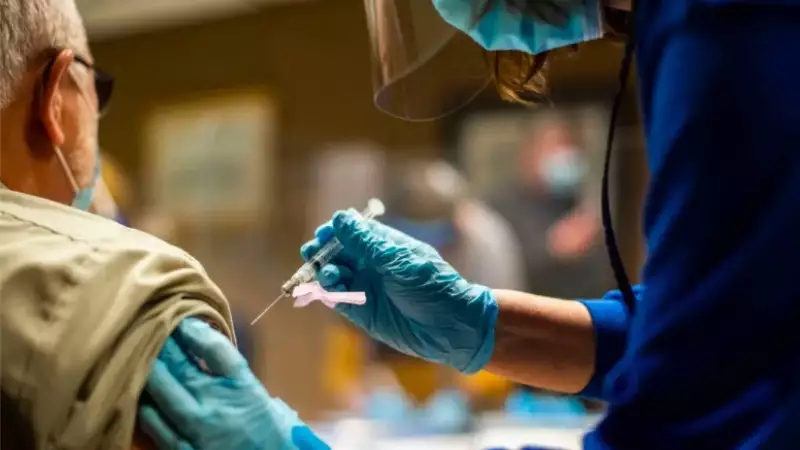
About the Call to Action
December 10, 2020 | A bipartisan assembly of Governors representing 1 in 3 Americans issued support for a historic Call to Action to Defeat COVID-19 and Promote National Recovery and Renewal, released by the COVID Collaborative.
This is the first time since the crisis began that Governors have come together on a bipartisan basis to support a common, comprehensive approach to defeating COVID-19 within and across states. In so doing, these Governors recognized that combating COVID-19 is a calling for the nation as a whole, and encouraged their fellow Governors to join them.
The recommendations in the Call to Action address the five key pillars of an effective response to COVID-19: testing, contact tracing, public health and social measures, vaccines and treatments, and common indicators of success. Across these pillars, it emphasizes the need for state and local leaders to engage with vulnerable communities, ensuring that efforts to defeat the virus are both equitable and effective.
The Call to Action integrates the very best science and practices on how to tackle the crisis, representing a public health consensus that transcends politics – a plan from the nation, for the nation.
FULL TEXT
A Call to Action to Defeat COVID-19 and Promote National Recovery and Renewal
Introduction
Earlier this year, America began the job of confronting a pandemic that has hit with the human cost of a war. In recent weeks, that cost has begun rising once again, as the level of new infections has reached new heights. We know from hard experience where we are headed without a dramatic change in course. More hospitalizations. More stress on our health system. More suffering among particularly vulnerable groups – the elderly, the ill and people in disadvantaged communities. And more needless deaths.
The question that comes to us has never been more urgent: Can a free and open society defend itself from an aggressively communicable disease?
We know the answer is “yes,” from the hard evidence of success. Across the country, we have seen front-line health workers perform wonders with a sense of duty stronger than fear. We have seen scientists energetically pursue vaccines and treatments for the benefit of Americans and all humankind. We have seen Americans care for themselves, families and neighbors. In all of this, we have witnessed the power of sympathy, generosity, compassion, public spirit, and simple goodness to one another.
Now is not the time for exhaustion, impatience or discouragement. While the challenge is on the rise, our knowledge of how to face it has increased as well. The lessons of this pandemic have been difficult. But at least they are clear.
We know that Americans must continue to broadly participate in their own rescue. Mask wearing, better hygiene and physical distancing gain power when they are practiced by everyone. The small, daily difference each person can make adds up to a very large difference in preventing the spread of COVID-19. We go up or down together, as one people.
We also know that the clarity and cooperation of government institutions at every level are essential. Americans must be given the facts, tools, inspiration, direction, and confidence to make their own efforts. We have also seen that no state or region can ultimately succeed alone. Spread of the virus in one state threatens all states. Defeating that threat is a calling for the nation as a whole.
America needs a consistent, coherent, cross-state approach to overcoming this disease. The outlines of an effective, common effort are not a mystery. Beneath the shifting waves of politics, there are deep currents of public health consensus. What we offer in this document is a description of that consensus, representing the collective wisdom of experts and implementers.
This consensus has five key pillars:

Testing
Defeating COVID-19 requires a redoubled commitment to testing. Without broad access to testing, our common response is flying blind. Only testing enables states to identify who has COVID-19, to prevent the disease from spreading in at-risk populations, and to predict where it is likely to go next;

Contact Tracing
Defeating COVID-19 requires strong contact tracing capabilities. Without tracing, small outbreaks easily gather into surges. Only tracing allows states to break chains of transmission before they grow to threaten lives and disrupt economic recovery;

Public Health and Social Measures
Defeating COVID-19 requires continued, widespread practice of public health and social measures. Masks, improved hygiene and physical distancing are our main tools to slow the spread of the disease and save lives;
Vaccines and Treatments
Defeating COVID-19 will require safe and effective vaccines and treatments. Without unprecedented federal, state, and local collaboration based on science, it will be difficult to extend a reliable distribution and tracking system to all communities across the country. And only such a system can properly stage the distribution of vaccines so the highest-risk groups are covered first; and
Common Indicators of Success
Defeating COVID-19 will require robust data and common indicators of success. Only good information and indicators can properly guide critical decisions on school openings and relaxing or imposing public health restrictions on businesses. And only clear performance indicators will allow us to continually improve testing and contact tracing.
This consensus has no agenda except the safety of the public. It reflects experience rather than ideology. For that reason, we believe that it can be the basis for the broadest, most effective campaign to halt the advance of COVID-19, and eventually get beyond it.
After Pearl Harbor, during World War II, there was a common phrase: “We are in it for the duration.” During a different kind of attack, that commitment endures. With cases surging, now is not a time for complacency, defeatism or needless division. In a pandemic, it is not possible to stand still. We will move ahead, or we will lose ground. Moving forward will require leadership, clarity and the united effort of a free people.
This Call to Action represents just such an effort, with recommendations developed by a national bipartisan assembly of leading experts and institutions. Implemented across state and party lines, these recommendations can hasten the day when every American can breathe safely once again; foster a unified effort and strong federal-state cooperation needed to defeat COVID-19; and put us on a path to a safer, more sustainable, and more prosperous America:

Testing
Implement an effective testing strategy within and across states to decrease viral transmission, reduce COVID-19 impacts, and enable schools, nursing homes, workplaces, hard-hit communities, and other at-risk settings to operate more safely and sustainably by:
Ensuring effective and comprehensive state COVID-19 testing action plans by:
- Implementing state testing programs with defined expectations for diagnostic tests (linked to contact tracing), screening tests (for people at risk of spread but without symptoms), and surveillance tests (to track viral activity).
- Prioritizing testing and support for populations experiencing a disproportionate burden of COVID-related morbidity and mortality.
- Providing ongoing and transparent communication with the public about the importance of testing and contact tracing to reduce spread.
- Establishing cross-state initiatives to enhance each state’s testing efforts by sharing data, best practices, capabilities, testing resources, and surge capacities.
Strengthening lab-based testing systems to ensure highly accurate diagnostic tests are available for those who need them, with a goal of returning results within 24 hours by:
- Prioritizing availability and use of PCR diagnostic tests to diagnose symptomatic individuals and their contacts, and other suspected cases.
- Coordinating with clinical laboratories, the federal government, and manufacturers to address supply chain shortages that limit testing (e.g., pipettes, reagents, approved swabs).
- Implementing payment and performance reporting mechanisms that reward timely and accurate results.
Expanding access to rapid screening tests in at-risk workplaces, shared-living facilities, schools, and neighborhoods by:
- Working in collaboration with these institutions and communities to deploy screening tests to help reduce viral transmission.
- Coordinating planning and distribution of tests provided through both state and federal mechanisms to ensure reliable supply and avoid shortages.
- Piloting testing initiatives and screening protocols, reporting on their impacts, and building the evidence base to scale the most effective practices.
- Expanding the use of the existing 10-state procurement compact to accelerate the introduction and supply of rapid point-of-care tests for all states.
- Requesting test manufactures and the federal government to work together to increase the number of rapid screening tests officially authorized for asymptomatic surveillance testing.
- Expanding capacity for pooled PCR tests for screening purposes through recruitment of academic labs, adoption of best practices, and reliable oversight of test performance and result reporting.
Working within and across states, and with the federal government and the private sector, to expand sustainable financing for COVID-19 testing by:
- Expanding coverage of COVID-19 diagnostic testing and related services for the uninsured, underinsured, and others with gaps in coverage through private insurers, federally-funded health programs, and state-supported programs.
- Requesting additional federal funding for states to purchase tests and supplies needed to execute a comprehensive strategy that includes screening and surveillance testing.
- Advocating for increased federal funding through grants, pre-purchase, or other mechanisms to bring rapid, accurate, lower cost, more convenient tests to market, and to scale up production of new and existing tests.
Strengthening public health surveillance systems to improve the reporting and utilization of testing data by:
- Establishing reliable systems for standardized reporting into public health surveillance systems of all diagnostic, point-of-care screening, and surveillance test results (both positive and negative).
- Ensuring timely reporting of positive results to appropriate health authorities, employers, schools, congregate living facilities, and individuals at home to allow for a prompt response.

Contact Tracing
Build a robust contact tracing capability to prevent and contain outbreaks by:
Ensuring adequate contact tracing capacity and adapting strategies based on the status of the pandemic by:
- Expanding and maintaining contact tracing capacity at a level sufficient to: 1) interview at least 80 percent of positive cases within 24 hours and identify and reach their contacts within 48 hours of a positive test result; and 2) conduct daily follow-up with contacts under quarantine through personal interaction and/or technological approaches.
- Recognizing that contact tracing efforts are likely to be much less effective when there are more than 10 cases per 100,000 population per day, and that in such a situation the key to gaining control of an epidemic is strengthening policies around masking, discontinuation of higher risk activities, and physical distancing.
- Acknowledging that when incidence levels are high, the focus of case investigation and contact tracing programs may need to shift toward large clusters and highest risk settings until incidence returns to a manageable level.
Ensuring adequate support for people in isolation and quarantine by:
- Establishing robust wraparound services to support people in quarantine and isolation by incorporating, for example, resource coordinators, care packages, timely links to healthcare, and financial support into contact tracing programs.
- Encouraging employers to provide paid leave for workers who need to quarantine at home because of exposure to a COVID-19 positive person.
Improving the effectiveness of contact tracing efforts by:
- Employing local individuals – especially those from vulnerable communities – as contact tracers and partnering with trusted community leaders to better understand community needs and improve the effectiveness of contact tracing.
- Using data collected during case investigations and contact tracing to determine high risk settings and activities, and transparently reporting such anonymized data online so that individuals and organizations can make more informed decisions about risk.
- Measuring and reporting each week on, at a minimum, the percentage of cases interviewed for contact elicitation in 24 hours from a positive test result, and the percentage of contacts reached within 24 hours of elicitation.
- Considering adoption of other key performance indicators, including the percentage of contacts under quarantine who complete the quarantine period; the number of contact tracers employed in a state or local jurisdiction; and the percentage of cases arising from quarantined contacts.
- Sharing best practices and innovations through an inter-state knowledge exchange platform so that states can learn from each other's successes and challenges.

Public Health and Social Measures
Promote implementation of proven public health measures for the general public to reduce the risk of community spread, and protect our families, neighbors, and communities by:
Promoting personal measures to reduce disease transmission by:
- Advocating for hand washing, physical distancing, and mask wearing through a multifaceted communications campaign to prevent the spread of SARS-CoV-2, with a special focus on engaging communities most affected by the pandemic.
- Implementing mask wearing measures, including mask requirements and making masks available, in indoor public places, which are associated with a higher risk of transmission.
Establishing best practice environmental measures by:
- Ensuring that sector-specific (e.g. businesses, schools) guidance on environmental measures to reduce transmission, including enhanced cleaning and ventilation, is based on best practice guidance from CDC and OSHA and made publicly available.
Engaging communities effectively on public health measures by:
- Developing and implementing across states a standardized phased risk-alert level system with associated sector-specific guidance for the general public and businesses at the state and county levels.
- Establishing, when appropriate, and clearly communicating evidence-based travel policies and associated control measures.
- Continuing to support public health measures until there is a very low level of community transmission, irrespective of vaccine availability.
Protecting the most vulnerable populations by:
- Implementing comprehensive infection control strategies in nursing homes and long-term care facilities as well as homeless shelters, correctional facilities, and locations such as meat-packing factories, which have been found to facilitate explosive spread of SARS-CoV-2.
- Facilitating and partnering with relevant stakeholders to ensure that there is adequate PPE for at-risk and other populations, such as healthcare workers, essential workers, and other workers in high-risk settings.
- Developing cross-cultural communications to reduce collective risk with a special emphasis on reaching key groups, including the elderly, those with underlying health conditions, communities of color, low-income workers, immigrant communities, and those who are incarcerated.

Vaccines and Treatments
Enable, in partnership with the federal government and manufacturers, the timely development and use of safe and effective vaccines and treatments by:
Supporting science-based development of vaccines and treatments by:
- Working collaboratively with the federal government on a development process that:
- Provides evidence from clinical trials and other data that meet FDA’s rigorous standards for safety and effectiveness, and from public assessment by independent FDA and CDC advisory committees;
- Provides clarity to Governors and any expert groups they are working with on what they should expect and can monitor to ensure that the federal approval and guidance process is science based; and
- Clearly communicates the evidence and process for emergency authorization or approval of vaccines and treatments to inform state actions to provide access.
- Encouraging diverse populations to participate in vaccine and treatment trials by collaborating with communities, research institutions, health care providers, and manufacturers.
Communicating clearly with the public and collaborating stakeholders on vaccine and treatment use and community impact by:
- Providing credible evidence-based messages from trusted messengers on the safety and efficacy of approved vaccines and treatments, including potential benefits, risks, and appropriate use.
- Partnering with providers and community leaders in high-risk communities to build trust, address barriers to access, and respond to concerns.
- Building public trust though clear, transparent, and frequent communication with the public about plans for distributing new vaccines and treatments.
Partnering with federal, local, tribal, and territorial governments, health care providers, community organizations, and other stakeholders to inform distribution plans that promote equitable uptake of vaccines by:
- Developing a transparent public process for allocating initial vaccine supply to populations at highest risk, based on vaccine safety and effectiveness, health equity, and public health impact.
- Supporting coordinated, cross-agency vaccine distribution planning that engages experts, healthcare providers, community leaders, and representatives from high-risk communities to inform state and local plans for distribution, access, and community engagement.
- Addressing critical operational details, such as recruiting and supporting vaccine providers, implementing tracking systems, storage of vaccines, and planning for supply.
- Eliminating financial barriers, such as copays for vaccine administration, for anyone who has difficulty paying.
- Advocating for adequate federal funding for state and local governments to execute distribution plans.
Partnering with key stakeholders to promote equitable access to and distribution of new treatments by:
- Planning for and supporting adequate manufacturing to meet patient needs.
- Crafting coordinated plans for initial distribution of new treatments, including monoclonal antibodies, that include targets for those patients with the highest need.
- Collaborating with the federal government and local public health authorities to assure timely and equitable access to monoclonal antibodies and other treatments after an emergency use authorization.
- Ensuring access to needed treatments, regardless of ability to pay.
Tracking use and monitoring safety and effectiveness of vaccines and treatments in collaboration with federal, state, local, and private sector entities by:
- Strengthening existing state data systems to track and monitor who gets the vaccine, ensure provider enrollment, manage ordering and vaccine inventory, enable timely reporting of data to federal partners, and integrate state-collected data with FDA- and CDC-supported platforms to identify serious adverse events.
- Collecting data on who receives new treatments, relevant side effects, and outcomes of new treatments to develop better evidence.
- Supporting timely reporting and analysis of post-market evidence on safety and effectiveness to inform and update vaccine and treatment distribution plans and public communications.
- Using data on vaccine and treatment uptake and impact in local populations to inform and refine access strategies and future actions, especially for higher-risk populations.

Common Indicators of Success
Enable evidence-based decision making through standardized indicators, measurable targets, and common thresholds for action by:
Promoting the use of standardized indicators to assess progress in the public health response to COVID-19 by:
- Collecting and reporting data publicly on essential indicators for tracking progress, such as those detailed in Exhibit A.
- Collecting and stratifying data by geography (to the most granular level possible), age, race and ethnicity, and underlying health conditions when possible.
- Collecting and reporting data from childcare facilities, K-12 schools, carceral facilities, and nursing homes/long-term care facilities, regarding infections and transmission of the SARS-CoV-2 virus within those environments.
Helping leaders make better-informed decisions about how to safely and sustainably reopen schools and businesses by:
- Adopting measurable indicators and targets.
- Seeking alignment of these indicators and targets across states, territories, tribes, and local jurisdictions.
Review and Implementation
Facilitate the implementation of the foregoing recommendations within and across states by:
- Working through a cross-state alliance to share best practices and information, optimize testing and contact tracing capabilities, help coordinate deployment of vaccines and new testing innovations, and promote public health measures and common indicators of success.
- Assessing these recommendations and their implementation, as circumstances evolve, not later than three months from the date hereof.
Together, we can win the battle against COVID-19 and build a safer, stronger, and more prosperous America.